Filter
1515
Filtered Results: 1515
Text search:
multilateral
Featured
Recommendations
73
New Publications
393
Language
Document type
No document type
756
Studies & Reports
407
Strategic & Response Plan
134
Guidelines
89
Manuals
68
Fact sheets
30
Situation Updates
13
Training Material
8
Resource Platforms
6
Brochures
2
Infographics
2
Countries / Regions
Global
152
Congo, Democratic Republic of
41
Africa
37
Ethiopia
35
Sierra Leone
33
Kenya
32
Latin America and the Carribbean
31
Nigeria
27
Liberia
25
Venezuela
24
Uganda
23
Zambia
23
Myanmar / Burma
22
Senegal
21
Malawi
21
Nepal
20
Benin
20
Syria
20
Mozambique
20
Rwanda
19
Germany
18
West and Central Africa
18
East and Southern Africa
17
Central African Republic
17
India
17
Ukraine
16
Guinea
15
Cambodia
15
Western and Central Europe
15
Burkina Faso
14
Haiti
14
Namibia
14
Indonesia
14
Lesotho
13
Middle East and North Africa
13
Ghana
12
Colombia
11
Tanzania
11
Brazil
11
Asia
10
South–East Asia Region
10
Bangladesh
10
South Sudan
10
South Africa
9
Yemen
9
Madagascar
9
Zimbabwe
8
Philippines
8
Cameroon
7
Peru
7
Moldova
7
China
5
Eastern Europe and Central Asia
5
Vietnam
5
Angola
5
Botswana
5
Thailand
4
Chile
4
Laos
4
Guinea-Bissau
4
Paraguay
4
Bolivia
4
Argentina
4
Lebanon
4
Eastern Europe
4
Mali
4
Ecuador
4
Pakistan
4
Tajikistan
3
El Salvador
3
Niger
3
Turkmenistan
3
Russia
3
Sudan
3
Timor Leste/ East Timor
2
Mexico
2
Togo
2
Iran
2
Uzbekistan
2
Afghanistan
2
Burundi
2
Malaysia
2
Hungary
2
Jordan
2
Western Pacific Region
2
North America
2
Jamaica
2
Japan
2
Spain
2
Côte d’Ivoire / Ivory Coast
2
Georgia
2
Poland
2
Honduras
2
Somalia
2
Eswatini/ Swaziland
2
Serbia
1
Gambia
1
Kazakhstan
1
Singapore
1
Kyrgyzstan
1
Congo-Brazzaville
1
Mauritania
1
Italy
1
USA
1
Croatia
1
Uruguay
1
France
1
Mauritius
1
Portugal
1
Azerbaijan
1
Belarus
1
Bosnia and Herzegovina
1
Papua New Guinea
1
Nicaragua
1
Sri Lanka
1
Egypt
1
Romania
1
Palestine
1
Libya
1
Bhutan
1
Guatemala
1
Authors & Publishers
Publication Years
Category
Countries
620
Key Resources
112
Public Health
66
Women & Child Health
45
Clinical Guidelines
32
Capacity Building
7
Pharmacy & Technologies
4
Toolboxes
COVID-19
145
Health Financing Toolbox
135
Planetary Health
103
HIV
96
Global Health Education
74
Conflict
62
Mental Health
60
TB
46
Disability
40
AMR
36
Refugee
35
Rapid Response
32
Ebola & Marburg
30
Natural Hazards
19
NTDs
17
Caregiver
16
Polio
11
Specific Hazards
10
Pharmacy
9
Social Ethics
7
NCDs
7
Malaria
6
Cholera
4
To deliver on the Global Fund Strategy milestones
for 2028 and ensure we keep the SDG 3 target
within reach, we need to raise US$18 billion to
fund the Global Fund’s next three-year grant cycle.
Si queremos cumplir los hitos de la Estrategia del Fondo
Mundial para 2028 y mantener a nuestro alcance la
meta del ODS 3, necesitamos recaudar 18.000 millones
USD para financiar el próximo ciclo de subvenciones
trienal del Fondo Mundial.
Overall, harmonisation and innovation should be the
focus of the future direction of DAH and the creation of
a healthy global community. The world needs all hands
on deck if it were to move towards achieving the SDGs,
addressing global health inequalities and improving the
welfare of the global...
The relative priority received by issues
in global health agendas is subjected to impressionistic
claims in the absence of objective methods of assessment
of priority. To build an approach for conducting structured
assessments of comparative priority health issues receive,
we expand the public ...
IHME’s Financing Global Health report provides an overview of health spending around the world, with a special focus on investments in health in low- and middle-income countries. The report examines how this funding for health is changing each year and forecasts how it may change in the future. Fi...
En su condición de departamento técnico de la OMS para el paludismo, al Programa Mundial sobre Malaria le corresponde una importante función de liderazgo de la respuesta mundial. Por medio de sus acciones directas y su red, tiene la capacidad de conformar el ecosistema de la respuesta al paludism...
Africa’s health sector is facing an unprecedented financing crisis, driven by a sharp decline of 70% in Official Development Assistance (ODA) from 2021 to 2025 and deep-rooted structural vulnerabilities. This collapse is placing immense pressure on Africa’s already fragile health systems as ODA ...
Zambia is facing a severe economic crisis marked by high inflation, increasing poverty and a heavy debt burden that is straining both its fiscal stability and progress in health outcomes. By 2020, the country's external debt reached United States dollars (USD) 12.7 billion, representing 108% of the ...
The Council was established in late 2020 by Dr Tedros Adhanom
Ghebreyesus (Director-General, WHO) to provide new economic thinking – reassessing how health and wellbeing are valued, produced and distributed across the economy. An all-female group of 10 distinguished economists and area experts, t...
For this report, the Task Force commissioned
additional background papers on health taxes to
update the evidence, assess short-term revenue
potential, and understand the role of health taxes
in the current era of multiple crises. We find that
health taxes continue to be underutilized despite th...
There has never been a more critical moment to invest in WHO, and strengthen the unique role it plays in global health. Now is the time to sustainably finance WHO and invest in a healthy return for all.
This Guide is part of WHO’s overall programme of work on Political Economy of Health Financing Reform: Analysis and Strategy to Support UHC. The impetus for this work came from demands for more concrete evidence, recognition and integration of political economy issues within
health financing, and...
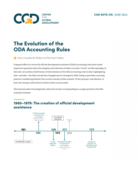
Frequent efforts to revise the official development assistance (ODA) accounting rules have raised important questions about the integrity and relevance of what currently “counts” as ODA spending. In this note, we outline a brief history of the evolution of the ODA accounting rules to date, highl...
The Plan of Action for Malaria Elimination 2021-2025 has been developed in consultation with countries and regional partners as a framework of reference to guide the efforts of countries and the contributions of donors and partners towards elimination of the disease in the Americas. The Plan subscri...
ndependent of the current conflict, the health sector in Ukraine faces several critical shortcomings. In particular, the country has an oversupply of hospitals and an undersupply of primary care and diagnostic facilities. Addressing these limitations will require substantial amounts of capital inves...
En la actualidad, los daños que sufren los pacientes a causa de una atención poco segura constituyen un desafío
importante y creciente para la salud pública mundial y son una de las principales causas de muerte y discapacidad
en todo el mundo. La mayor parte de estos daños son evitables. Ahor...
Self-care interventions are among the most promising and exciting new approaches to improve health and well-being, both from a health systems perspective and for people who use these interventions.
The World Health Organization (WHO) uses the following working definition of self-care: Self-care i...
síntesis de hallazgos en cinco países de América Latina
Das Dokument soll dem Erkennen, Bewerten und Bewältigen des Auftretens von Ebolafieber in Deutschland dienen und richtet sich dabei primär an den öffentlichen Gesundheitsdienst sowie medizinisches Fachpersonal in der klinischen, ambulanten und rettungsdienstlichen Versorgung in Deutschland. Es is...