Filter
7643
Filtered Results: 7643
Text search:
contributions
Featured
Recommendations
580
New Publications
1969
Language
Document type
No document type
4142
Studies & Reports
1628
Guidelines
795
Manuals
397
Strategic & Response Plan
337
Training Material
136
Fact sheets
101
Situation Updates
58
Brochures
17
Resource Platforms
15
Infographics
9
Online Courses
5
Dashboards/Maps
1
App
1
Videos
1
Countries / Regions
Global
401
India
236
Kenya
210
Ethiopia
167
Uganda
150
Nigeria
138
Sierra Leone
137
Latin America and the Carribbean
134
South Africa
133
Nepal
132
Myanmar / Burma
124
Senegal
122
Malawi
118
Congo, Democratic Republic of
118
Africa
116
Liberia
109
Tanzania
107
Rwanda
105
Zambia
101
Western and Central Europe
95
Ghana
89
Burkina Faso
85
Bangladesh
83
Benin
76
Namibia
72
Syria
69
Ukraine
63
Guinea
63
Haiti
61
Philippines
54
Zimbabwe
48
Cambodia
47
South Sudan
45
Cameroon
44
Lesotho
42
Mozambique
41
Central African Republic
40
Venezuela
39
West and Central Africa
39
Asia
38
Indonesia
38
South–East Asia Region
37
Eastern Europe
37
Madagascar
31
East and Southern Africa
30
Middle East and North Africa
27
Mali
27
Brazil
25
Botswana
25
Germany
24
Colombia
23
Pakistan
22
Yemen
21
Côte d’Ivoire / Ivory Coast
20
Russia
19
Afghanistan
18
Paraguay
18
Niger
17
Lebanon
17
Jordan
16
Eastern Europe and Central Asia
16
Thailand
15
Eswatini/ Swaziland
15
Peru
14
Somalia
14
Togo
13
Burundi
12
Vietnam
12
Sri Lanka
12
Sudan
11
China
10
Iraq
10
Tajikistan
9
Chile
9
Laos
9
USA
9
Western Pacific Region
9
Moldova
9
North America
8
Southern Africa
8
Iran
7
Albania
7
Argentina
7
Chad
7
North Macedonia
6
Turkey
6
Kyrgyzstan
6
El Salvador
5
Egypt
5
Poland
5
Bhutan
5
Timor Leste/ East Timor
4
Mexico
4
Serbia
4
Gambia
4
Kazakhstan
4
Japan
4
Spain
4
Bolivia
4
Papua New Guinea
4
Georgia
4
Ecuador
4
Canada
3
Congo-Brazzaville
3
Malaysia
3
Morocco
3
Hungary
3
Jamaica
3
France
3
United Kingdom
3
Portugal
3
Bosnia and Herzegovina
3
Romania
3
Honduras
3
Angola
3
Libya
3
Switzerland
2
Fiji
2
Singapore
2
Estonia
2
Mauritania
2
Armenia
2
Dominican Republic
2
Guinea-Bissau
2
Croatia
2
Turkmenistan
2
Tunisia
2
Israel
2
Djibouti
2
Palestine
2
Guatemala
2
Uzbekistan
1
Vanuatu
1
Mongolia
1
Qatar
1
Bulgaria
1
Italy
1
Lithuania
1
Ireland
1
Saudi Arabia
1
Luxembourg
1
Belgium
1
Mauritius
1
Norway
1
Morocco
1
Azerbaijan
1
Belarus
1
Guyana
1
Slovakia
1
Greece
1
Authors & Publishers
Publication Years
Category
Countries
2909
Key Resources
474
Clinical Guidelines
455
Public Health
424
Women & Child Health
380
Capacity Building
139
Pharmacy & Technologies
55
Annual Report MEDBOX
2
Toolboxes
Mental Health
535
HIV
467
COVID-19
456
Planetary Health
401
TB
351
Disability
328
Caregiver
258
NTDs
240
Conflict
198
Ebola & Marburg
191
AMR
176
Health Financing Toolbox
173
Rapid Response
162
Global Health Education
154
NCDs
139
Refugee
126
Natural Hazards
106
Pharmacy
103
Malaria
101
Social Ethics
64
Zika
37
Specific Hazards
34
Polio
34
Cholera
31
2.0 Rapid Response
18
Typhoon
8
South Sudan
1
To deliver on the Global Fund Strategy milestones
for 2028 and ensure we keep the SDG 3 target
within reach, we need to raise US$18 billion to
fund the Global Fund’s next three-year grant cycle.
Pour franchir toutes les étapes de la stratégie du
Fonds mondial jusqu’en 2028 et nous assurer que la
cible de l'ODD 3 reste à notre portée, nous devons
mobiliser 18 milliards de dollars US pour notre prochain
cycle triennal de subvention.
The role of evidence in the journey towards universal health coverage is paramount. Financial risk protection monitoring, the major focus of this report, informs where the WHO African Region stands in reducing the financial hardship people face due to health expenses. This report details the status ...
As part of the project ‘Equitable health financing for a strong health system in Mozambique’, N’weti and Wemos developed this policy brief with actionable policy recommendations for the Mozambican government and international organizations on how to increase resources for health in a sustainab...
Over the past decade, countries in the African region experienced slow progress in mobilizing resources for health while facing continued challenges. In their revised estimates published in 2017, Stenberg et al., developed two costs scenarios, termed progress and ambitious, aimed at strengthening co...
The relative priority received by issues
in global health agendas is subjected to impressionistic
claims in the absence of objective methods of assessment
of priority. To build an approach for conducting structured
assessments of comparative priority health issues receive,
we expand the public ...
IHME’s Financing Global Health report provides an overview of health spending around the world, with a special focus on investments in health in low- and middle-income countries. The report examines how this funding for health is changing each year and forecasts how it may change in the future. Fi...
This paper presents a bibliometric analysis of the literature on private health aid and official health assistance between 2000 and 2022. It provides an overview of the sites and themes in the literature pertaining to development assistance in health, and collates the significant policy recommendati...
Each year since 2007, G-FINDER has provided policy-makers, donors, researchers and industry with a comprehensive analysis of global investment into research and development of new products to
prevent, diagnose, control or cure neglected diseases in low- and middle-income countries, making it the go...
Africa’s health sector is facing an unprecedented financing crisis, driven by a sharp decline of 70% in Official Development Assistance (ODA) from 2021 to 2025 and deep-rooted structural vulnerabilities. This collapse is placing immense pressure on Africa’s already fragile health systems as ODA ...
Development assistance for health (DAH)
plays a vital role in supporting health programmes in lowand middle-income countries. While DAH has historically
focused on infectious diseases and maternal and child
health, there is a lack of comprehensive analysis of DAH
trends, strategic shifts and the...
The Council was established in late 2020 by Dr Tedros Adhanom
Ghebreyesus (Director-General, WHO) to provide new economic thinking – reassessing how health and wellbeing are valued, produced and distributed across the economy. An all-female group of 10 distinguished economists and area experts, t...
This comprehensive HPFM report thoroughly explores Kenya’s health financing landscape. It provides an in-depth analysis of the current state of affairs and sheds light on required strategic changes in health financing. The report points out the need to improve public financial management within th...
The COVID-19 pandemic exposed critical gaps in the global response to health crises, particularly in the financing of pandemic prevention, preparedness, response, recovery, and reconstruction. This chapter presents a comprehensive framework for pandemic financing that spans the entire pandemic cycle...
Questions concerning the relevance and reform of official development assistance (ODA), and how ODA and broader development finance could—or should—change to better reflect shifting demands are not new, with academics and policymakers suggesting a range of options for reform. In this background ...
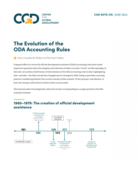
Frequent efforts to revise the official development assistance (ODA) accounting rules have raised important questions about the integrity and relevance of what currently “counts” as ODA spending. In this note, we outline a brief history of the evolution of the ODA accounting rules to date, highl...
The world is facing a sustainable development crisis. The 2024 Financing for Sustainable Development Report: Financing for Development at a Crossroads finds that financing challenges are at the heart of the crisis and imperil the SDGs and climate action. The window to rescue the SDGs and prevent a c...
The Plan subscribes to the goals and pillars of the WHO Global Technical Strategy against Malaria 2016-2030 (GTS), while presenting key elements to address the specific challenges of the Region.
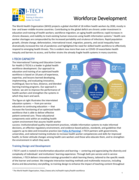
Technical Brief Workforce Development
recommended
The World Health Organization (WHO) projects a global shortfall of 18 million health workers by 2030, mostly in low- and lower-middle-income countries. Contributing to the global deficit are chronic under-investment in education and training of health workers; workforce migration; an aging health wo...
In 2008 the Ministry of Health and Social Services (MOHSS) commissioned a national health and social service system review which found that although some progress has been made in primary health care, provision of health services did not go beyond the health facilities, irrespective of the fast dist...